(Bio)engineered KidNey systems for blood detoxification
For patients with chronic kidney disease the best solution would be organ transplantation. However, due to shortage in donor organs and the fact that not all patients are eligible for transplantation, most patients are currently treated with therapies using artificial kidney devices. In hemodialysis, a widely available and well-established treatment for the patients with End Stage Renal Disease, the blood of these patients is cleansed 3-4 times a week in dedicated dialysis centres. Major drawbacks of the therapy are the poor removal of middle-sized molecules and protein-bound uremic solutes and the non-continuous treatment, causing large fluctuations in water balance and uremic wastes of the patients. Besides, the need for continuous visits at the dialysis centres is a great social and psychological burden for these patients.
The chair of (bio)artificial organs, led by Professor Dimitrios Stamatialis, focuses on developing bioengineered kidney systems for mimicking the kidney function in better ways, including:
- Artificial kidneys based on Mixed matrix membranes (MMM) which combine the benefits of diffusion and /or convection, provided by the membrane structure, and of adsorption, achieved by sorbent particles dispersed in the membrane (Figure 1, [1]). The MMM can be applied for removing a broad range of uremic toxins and can be implemented in a portable artificial kidney device.
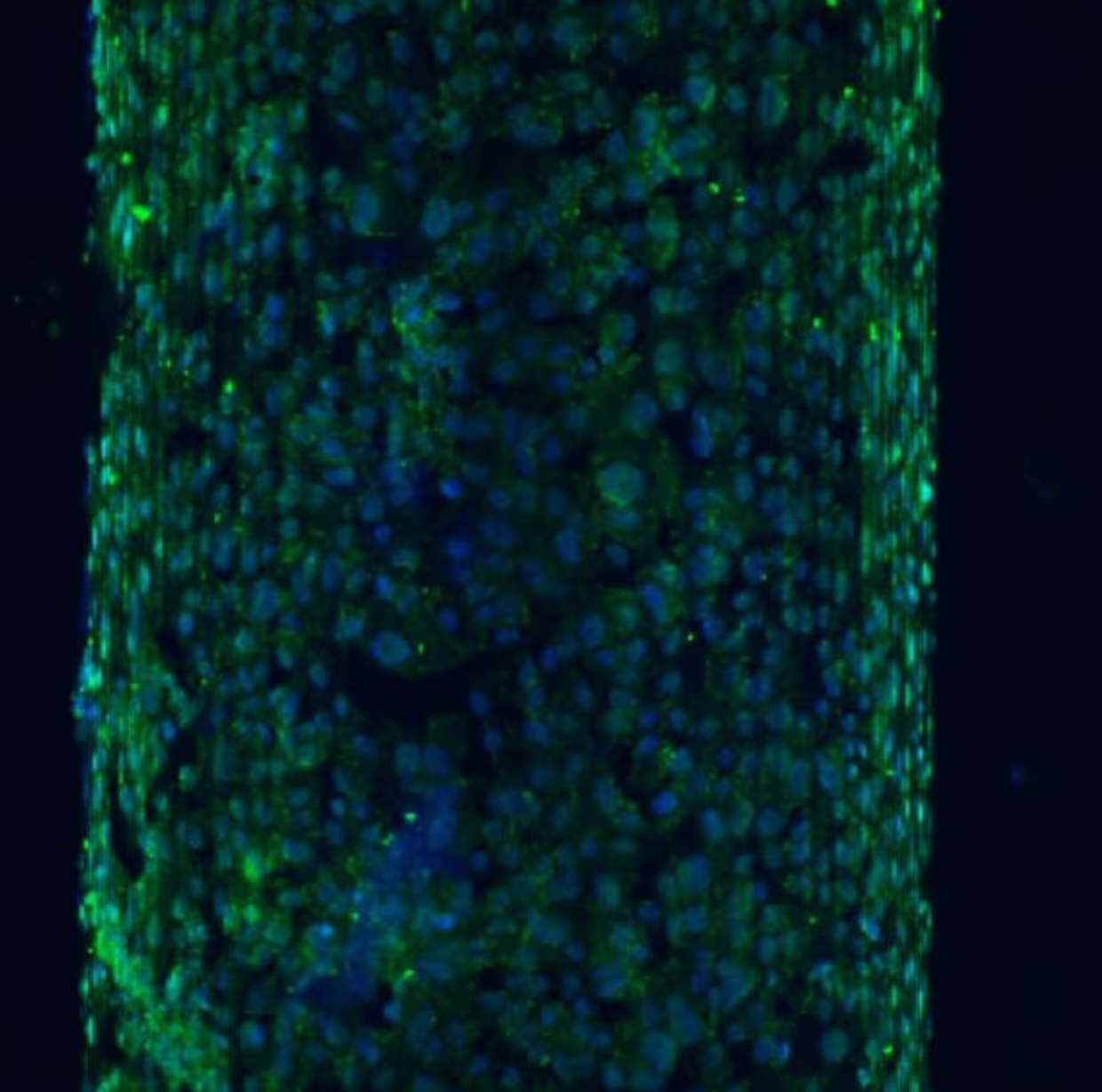
- Bioartificial kidney (BAK) where “living membranes” of tight renal cell monolayer with preserved functional organic ion transporters attached on suitable artificial membranes (Figure 2), can actively remove the uremic solutes, mimicking the function of the kidney proximal tubule.
Both MMM and BAK systems can be applied for removing a broad range of uremic toxins and could be implemented in a portable (bio)artificial kidney devices.