Functional Individual Tailor-made Upright Pessaries
PROJECT ACRONYM
FIT-UP
FUNDED BY
NWO-OTP
PHD CANDIDATE
WP 1 (Functionality and Multimodality Imaging and Sensing): Vacancy
WP2: Development of Instrumented Pessaries (IPs) by 3D printing: Dimitris Kosmas
POSTDOC RESEARCHER
WP3: Finite Element Modelling: Frieda van den Noort
SUPERVISORS
Promotor: Srirang Manohar
Co-promotor: Frank Simonis and Anique Bellos-Grob
COLLABORATION
CLINICAL BACKGROUND
Pelvic organ prolapse (POP), a non-lethal but highly disabling disease, is characterized by a pelvic floor organ (e.g. bladder, uterus, bowel) protruding (prolapsing) from the opening of the vagina. Globally, up to 50% of all women who have had children have some degree of clinical POP and 10–20% are symptomatic; causing reduced participation in society, reduced workforce and a lower quality of life. The main treatment options for POP are conservative treatment with a pessary or surgical correction. A pessary is a ring shaped device, usually made from silicone, that when inserted into the vagina, aims to provide mechanical support to hold up the prolapsed tissues above the pelvic floor. However there are two major limitations in current conservative POP treatment. First, it is often necessary to try several pessaries before obtaining an adequate fit and second, when fitting is unsuccessful, surgery (with known high recurrences) is the only treatment option left. The mechanical performance of current pessaries during and after implantation remains poorly understood. Unsuccessful fitting is described as pessary dislodgment, discomfort/pain, de novo and failure to relieve POP symptoms. International studies concluded that the percentage of women who continue wearing the pessary after one year is only around 60-68%. We hypothesize that successful fitting is related to the size and shape of a pessary. Therefore, we want to better understand the interaction between anatomy and pessary to implement this knowledge in a specialized medical device. Furthermore, we want to improve pessary fitting and therapy by developing a personalized method (and in time device) by tailoring it anatomically and functionally to an individual. This calls for a smart combination of innovative technologies:
- Functionality and Multimodality Imaging and Sensing (FMIS): to better understand the pelvic floor functionality in relation to wearing a pessary, multiple medical imaging and sensing modalities (ultrasound (US), Magnetic Resonance Imaging (MRI), EMG) will be deployed to get detailed anatomical information and muscle mechanics.
- Development of an Instrumented Pessary (DIP): To enable research on personalized pessaries, improved pessary imaging (using registration marks on the pessaries) and sensing of force and pressure on the pessary in vivo, a pessary with functionality sensors for research purposes will be designed and fabricated by 3D printing.
- Finite Element Modelling (FEM): A detailed patient-specific computational platform will be developed using advanced finite element modelling techniques and optimization of data acquisition techniques. This platform will enable personalized pessary design for better treatment outcomes.
POP heavily impacts patients’ quality of life, but remains a small research area in relation to other women’s health topics. In short, the treatment options are based on outdated technologies and the field is craving for more tailor made solutions. We believe that functional imaging and advanced materials are the way to reduce costs and improve POP treatment. The integrated knowledge and technology development from the three proposed research lines will enable understanding of the failure of pessaries, insights into requirements of a personalized device, and first steps in realization of prototypes of personalised-fit pessaries.
OBJECTIVE
The most important aspect for a proper pessary fitting is a good match between the pelvic floor (anatomy and functionality) and the size, shape and tissue of the pessary. To develop a method which leads to better fit a pessary three highly integrated work packages (WP) are identified:
1. Functionality and Multimodality Imaging and Sensing (FMIS)
2. Development of Instrumented Pessaries (sensors) (DIPs)
3. Finite Element Modelling (FEM)
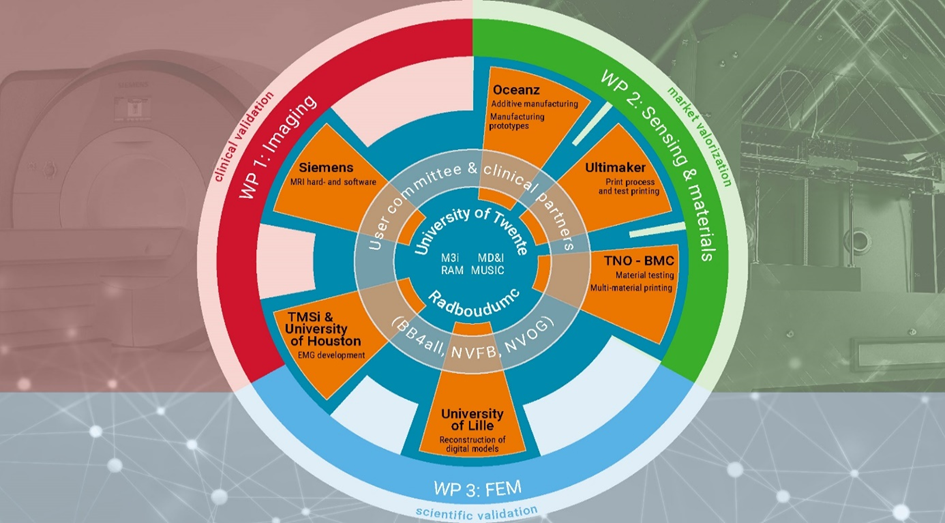
The scientific work in this project (UT in collaboration with Lille and Houston) is accompanied by clinical (BB4all, NVOG, NVFB) and industry commitment (Oceanz, Ultimaker, TNO Brightlands, TMSi, Siemens Healthineers) to enable to project outcome valorization. This collaboration, added value and commitment per partner in this project is visualized in Figure 3. It is not our (primary) intent to work towards large scale fabrication of (customized) pessaries but rather to obtain more accurate assessments of the fitting of specific pessaries for individual women. Moreover, we anticipate that ultimately, customized pessaries may be an affordable and relatively convenient way to improve pessary efficacy, reducing the need for surgical procedures.
PROJECT DETAILS
FIT-UP will start in May 2022
PUBLICATIONS
